Almost ten years after a young girl suffered a life-threatening reaction to the children’s pain reliever, Motrin, that caused her to lose most of her skin and left her legally blind, Johnson & Johnson was ordered to pay $63 million to the girl and her parents.
In 2003, when the then-7-year-old girl from Plymouth, Massachusetts, had a fever, her parents gave her Children’s Motrin. The girl had previously taken Motrin without suffering any side effects. However, this time, instead of her condition improving, she got worse, and ended up in the hospital for months. More specifically, the disease inflamed the girl’s throat, mouth, eyes, esophagus, intestinal tract, respiratory system, and reproductive system, forcing physicians to put her in a coma. Unbeknownst to her parents, ibuprofen, a common painkiller found in Motrin, can cause a rare, and potentially fatal, skin disease known as toxic epidermal necrolysis or “TEN” that eats away at your skin.
The young girl was not only forced to undergo surgery to drill through her skull to relieve some pressure, but she also lost 90% of her skin and is now legally blind. In addition, the girl suffered severe permanent lung and liver damage, and now has only 20% lung capacity. Although she also suffered brain damage, it caused only short-term memory loss.
Following this grueling experience, in 2007, the girl’s parents sued Johnson & Johnson, the maker of Motrin, and its subsidiary, McNeil PPC, Inc., for failing to provide proper warning of the possible side effects. The key issue in the lawsuit was the warning label Johnson & Johnson used for Children’s Motrin, made by McNeil-PPC, Inc. Notably, even though the prescription version of adult Motrin briefly mentions Stevens-Johnson Syndrome, a more common version of TEN, the over-the-counter children’s version of Motrin that was provided to the young girl, contained no such warning at all.
A manufacturer can be sued under one of three theories for injuries caused by a product or drug, including: (1) defective design, (2) defective manufacturing, or (3) defective warning and labeling. Here, the family sued the health care company under the third theory, alleging that the company failed to meet its labeling requirement. When dealing with warning labels, courts can find a product defective because of an inaccurate or inadequate warning label. Importantly, by law, the manufacturer is required to warn consumers of hidden dangers, and instruct users how to use a product in a way that will avoid the dangers.
In this case, the jury agreed that Johnson & Johnson failed to provide adequate warnings about ibuprofen’s potential side effects and awarded the girl, now 16, $50 million, and awarded an additional $6.5 million to each of her parents. With interest, the award totals $109 million.
Continue reading →

 Texas Injury Lawyers Blog
Texas Injury Lawyers Blog



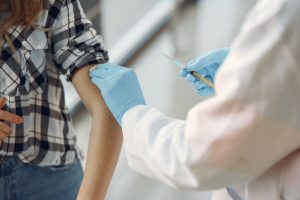 Vaccines are one of the most effective ways to prevent the spread of infectious diseases throughout the world. The overwhelming majority of people who receive vaccines do not experience serious problems, and the benefits greatly outweigh the threat of risk. However, similar to the risks associated with natural supplements and other pharmaceuticals, some vaccine recipients may suffer adverse reactions. Depending on the nature and circumstance of the injury, victims may file a Texas medical malpractice or pharmaceutical error lawsuit. Further, the National Vaccine Injury Compensation Program (VICP) provides compensation to individuals who have suffered injuries from certain vaccines.
Vaccines are one of the most effective ways to prevent the spread of infectious diseases throughout the world. The overwhelming majority of people who receive vaccines do not experience serious problems, and the benefits greatly outweigh the threat of risk. However, similar to the risks associated with natural supplements and other pharmaceuticals, some vaccine recipients may suffer adverse reactions. Depending on the nature and circumstance of the injury, victims may file a Texas medical malpractice or pharmaceutical error lawsuit. Further, the National Vaccine Injury Compensation Program (VICP) provides compensation to individuals who have suffered injuries from certain vaccines.